Utilizing Public Health to Address Elder Abuse
By Karon Phillips, Ph.D., MPH, CHES, Policy Development Manager and Megan Wolfe, JD, Senior Policy Development Manager at Trust for America’s Health
April 6, 2023

By 2030, one in five people will be aged 65 and over. With this incredible increase in longevity, it is important to make sure that the problems of today do not become the problems of tomorrow, and that new generations of older adults have the tools and resources they need to thrive and age healthily. Public health has shown great progress in addressing the needs of older adults, from programs relating to fostering healthy brains to Healthy People 2030 including as one of its goals to “improve health and well being for older adults.” The COVID-19 pandemic exposed the breadth of health challenges of older adults and underscored the need for public health attention to this growing population. One of those challenges that was exacerbated during the pandemic is elder abuse.
While there is limited data on the phenomenon—primarily due to underreporting—elder abuse is experienced by about one in 10 community-dwelling older adults each year. The COVID-19 pandemic created more opportunities for elder mistreatment with people sheltering in place and more isolated; at least 54% of calls to the National Center on Elder Abuse (NCEA) reported abuse during the first year of the pandemic, primarily physical and emotional (although this does not prove a causal link). Elder mistreatment can cause depression and keep older people from engaging with others. It has the potential to result in hospitalization or institutionalization. It has been shown to impact cognitive health and even cause premature death.
There are currently some public health resources that exist to address elder abuse, but they are limited. The CDC’s National Center for Injury Prevention and Control has a website that includes some prevention principles and resources for public health practitioners. But the resources available through the Injury Center are more broadly focused and not just on older adults. In addition, dedicated public health funding to address elder abuse is frequently inadequate, resulting in limited resources and support for public health engagement in this crucial area of concern.
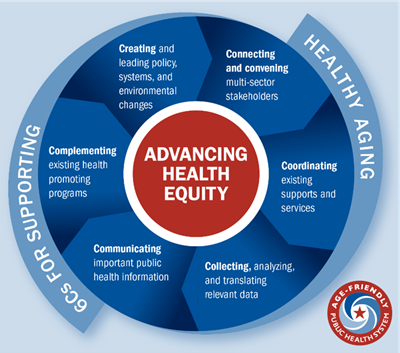
Elder mistreatment is a public health issue, but there is little guidance in how public health practitioners can prevent abuse and better support those who become victims. Trust for America’s Health, which leads the national Age-Friendly Public Health System movement, offers a framework (see graphic below) that describes roles and policies for public health practitioners to build capacity and develop programs for healthy aging.
The AFPHS 6Cs framework provides some valuable first steps for public health engagement in elder abuse.
- Create and lead policy and systems change: public health leaders can familiarize themselves and their colleagues on the health impacts of elder abuse and systemic factors that put older people at risk for abuse.
- Connect and convene community partners: public health practitioners can convene multi-sector partners, including older adults and their families, hospitals, pharmacies, emergency personnel, and the aging services sector to assess needs and target interventions.
- Communicate public health information and best practices: public health departments can use their messaging channels to highlight the risk factors, such as social isolation, as well as signs of elder abuse, and promote methods of reporting abuse.
- Collect and analyze data: public health practitioners can assess and identify indicators of elder abuse, and enhance data collection on risks, health impacts, and incidents of elder mistreatment.
- Coordinate existing services and supports: public health can identify and coordinate community screening services and help to improve access to existing services.
- Complement existing services and programs: once existing programs are identified, public health departments can work with community coalitions and other partners to create new ways to capture data, develop and deliver screenings, and ensure that all of their staff are well-positioned to recognize and address elder mistreatment.